Obesity surgery eclipses weight loss wonder drugs like Wegovy when it comes to saving lives, research shows.
The slimming jabs are in short supply due to unprecedented demand from those eager to copy celebrity users including Sharon Osbourne and Oprah Winfrey.
But a new study reveals they are less effective at preventing premature deaths among obese patients from weight-related illnesses such as heart disease, diabetes and cancer.
Around 7,000 people a year in the UK undergo obesity (bariatric) surgery.
To qualify on the NHS, body mass index must be 40 or higher.

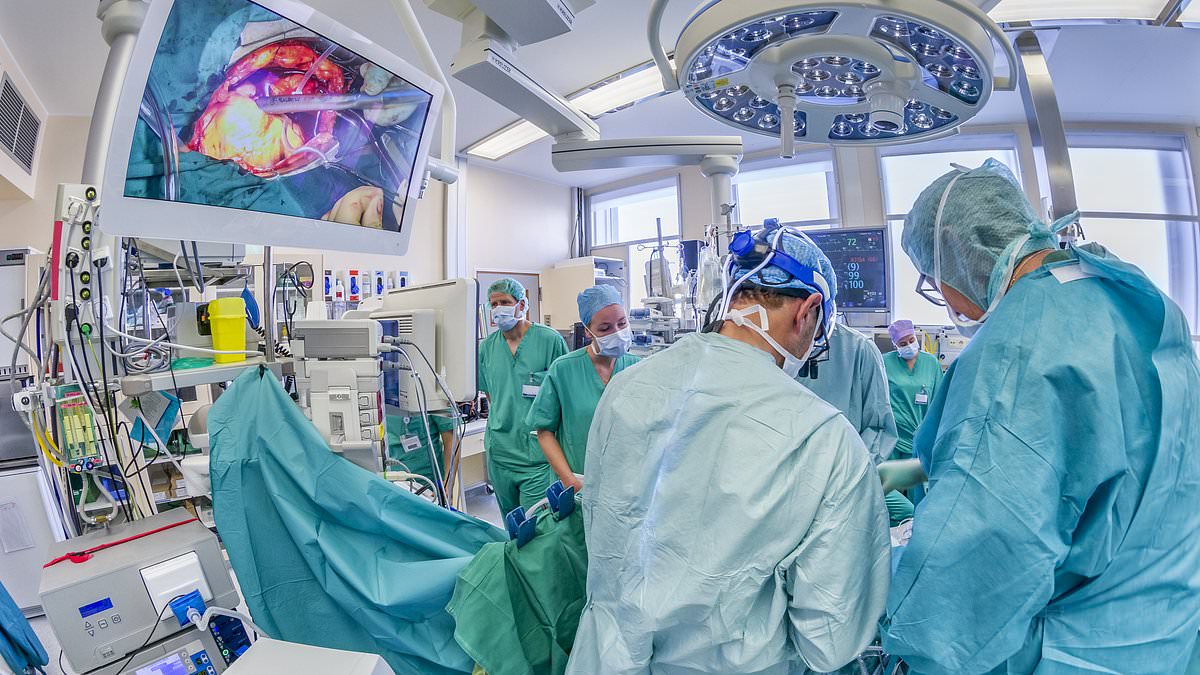
Scientists at Hasharon Hospital in Israel, suggest obesity surgery carries greater long-term benefits and is more effective at preventing premature death than weight-loss jabs

More than 6,000 obese patients, with an average age of 51, were tracked over six years in the study, which found those who had surgery were 62 per cent less likely to die from obesity-related health problems than those treated with Ozempic-style injections (file pic)
Surgeons make the stomach smaller, usually through a gastric bypass or by inserting a band, so that patients feel fuller sooner and eat less as a result.
The op, costing up to £15,000, requires a short stay in hospital. There has been speculation semaglutide-based obesity drugs – which mimic the effects of a hormone called GLP-1 that tells the brain the stomach is full – could reduce the need for gastric operations.
However, the latest study, by scientists at Hasharon Hospital in Israel, suggests surgery carries greater long-term benefits.
They tracked more than 6,000 obese patients, with an average age of 51, over six years and found those who had surgery were 62 per cent less likely to die from obesity-related health problems than those treated with Ozempic-style injections.
Researchers said the results, in the journal JAMA Open Network, reflected the fact that weight lost through surgery was greater than on the drugs.
Obese patients shed an average of 31 per cent of body weight with surgery while those on GLP-1 inhibitor drugs – which stop working if not taken for life – lost just 12.8 per cent.
‘The risk of death falls when patients lose more than 10 to 15 per cent of body weight,’ says Prof Alex Miras, consultant endocrinologist at Imperial College, London.
‘But the newest GLP-1 drugs help patients lose more, so ten years on, they may be equally effective as surgery.’